- What exactly is Long-Term Care?
- Long Term Care Defined
- Types of Long Term Care
- Long Term Care Settings
- The Cost of Long Term Care
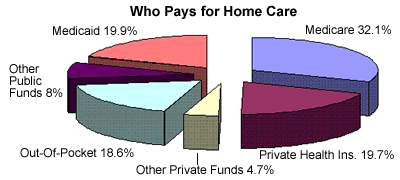
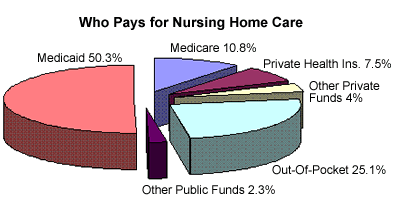
- Who pays for Long Term Care?
Generally, long-term care is the care people need when they can’t perform the tasks of ordinary living independently. It isn’t a subject that most of us care to dwell on. However, the failure to discuss or plan for the high cost of long-term care is causing American families to be unprepared to meet the high costs of long-term care. This section addresses what long-term care is and where it is provided, as well as the costs of long-term care and who pays for it.
Long-term care is the personal care and other related services provided on an extended basis to people who need help with activities of daily living or who need supervision due to a severe cognitive impairment. This type of care is considered skilled care, non-skilled care, or custodial care. It is NOT acute or rehabilitative care, which is known as skilled care.
When you need long-term care you usually need help with your activities of daily living. These are items such as bathing, dressing, toileting, continence, eating, and transferring. Or, you may be able to do all of your activities of daily living but still need care and supervision due to a severe cognitive impairment (memory loss, dementia, etc.). You may be able to dress yourself, but you may not remember to take your medications.
Nearly one-seventh of the nation’s current elderly population – an estimated 5.2 million – have a limitation in either activities of daily living (ADL), instrumental activities of daily living (IADL), or both. More than one-third of these have limitations in 2 or more ADLs.
Long-Term Care Insurance, Better Information Critical to Prospective Purchasers
United States General Accounting Office, September 2000
Acute Versus Chronic Care
Acute care is the type of care that is usually provided in hospitals and emergency rooms. Your health insurance and Medicare will likely cover some or all of the expenses for acute care because it is usually skilled care. Acute care is usually for conditions that are treatable and you may fully recover with the right medical attention. Acute care conditions usually develop rapidly and can strike suddenly. Examples of Acute Care: Stroke, heart attack, pneumonia
Chronic care is the type of care that is usually provided in your home, nursing homes, and assisted living facilities. Your health insurance and Medicare will usually not cover chronic care because it is not considered skilled care. Chronic care is usually for conditions that are treatable but generally not curable. A lot of times they are not noticed or are ignored in the initial stages. Examples of Chronic Care: Arthritis, Diabetes, Hypertension, Alzheimer’s
Skilled Care
Skilled care is the type of care that is usually delivered in skilled nursing homes, but can be received in the home as well. If the skilled care meets strict criteria set forth by Medicare, then the facility providing it is referred to as a skilled nursing facility (SNF). Medicare defines skilled care as services and rehabilitation that require the skills of technical or professional personnel such as registered nurses, licensed practical nurses, and physical or occupational therapists. Example: John recently had his hip replaced. Although he is expected to recover fully, he needs physical therapy to be able to walk again. He was admitted to a skilled nursing facility to receive his therapy. He will remain there as long as he needs therapy on a daily basis and is getting better.
Non-Skilled Care
Non-skilled care is defined as the type of care that is provided to persons who need help on a regular basis with their activities of daily living because of a physical limitation, chronic problem, or a cognitive problem. A family member can provide this type of care. It does not have to be performed by a medical professional like skilled care does. Non-skilled care is also known as custodial care. Example: Marge is suffering from rheumatoid arthritis. She has difficulty dressing herself and getting in and out of the bathtub. Her daughter comes to her house in the morning and evening to take care of her mother’s needs.
Long-term care can be received in a variety of settings. The setting is usually determined by your support system (your family, attending physician, or someone qualified to develop a plan of care) that you have and the reason that you need long-term care. Some needs can easily be taken care of at home, while others would be better cared for in a nursing home.
Skilled Nursing Facilities
The number of nursing home patients has actually declined in recent years due to an increased availability of home health and other community services.
Medical Deductions for the Elderly, Part II, Expenses and Premiums Related to Long-Term Care”, The ElderLaw Report, Panel Publishers, March 2002
Skilled nursing facilities are usually comprised of two separate components. The first component is a unit that provides skilled nursing care that may be covered by Medicare (if the care meets the criteria that Medicare sets forth). The rest of the facility provides non-skilled (or custodial) care. The goal of the “Medicare” section of the skilled nursing facility is to provide services needed to rehabilitate the patient so they can return home. However, many times patients are unable to return home and are moved over to the non-skilled or custodial section of the facility. Usually in these cases the patient may not have any support services or family in the community that would allow them to leave the facility. Example: Betty had a stroke 12 months ago. Immediately after her stroke she was admitted to a skilled nursing facility in the Medicare section and received rehabilitative therapy on a daily basis. After about 45 days, her therapists determined that she was not getting better and would need help with her activities of daily living for the rest of her life. Because she did not have anyone to take care of her at home, she was transferred to the non-skilled wing of the skilled nursing facility where she will live the rest of her life.
Home Care
Most people – nearly 79% – who need LTC live at home or in community settings, not in institutions.
Long-Term Care Users Range in Age and Most Do Not Live in Nursing Homes: Research Alert Agency for Healthcare Research and Quality, November, 2000
Home care is generally considered appropriate at the custodial and non-skilled care levels. Skilled care can be provided in the home, however it can be very expensive. Home care could consist of a weekly visit by a homemaker that performs housekeeping chores, a personal care attendant that provides assistance with bathing and dressing, or it may be a daily visit by a home health registered nurse or therapist. Example: Helen was diagnosed with Parkinson’s disease two years ago. Now she is unable to walk without assistance. She cannot bathe or dress herself. Her daughter, Donna, is currently helping her with these needs. Her daughter has to go back to work in order to save money for her two children that will be going to college in the next two years. Helen is now going to have to tap into her life savings and pay for a caregiver to come in and help her, instead of her daughter, so that she can stay at home.
Assisted-Care Living Facilities (ACLFs)
Between 1998 and 2000, the number of assisted living and board and care facilities increased from 24, 572 to 32,886 nationally reflecting the trend towards community-based care as opposed to nursing homes.
State Assisted Living Policy: 2000 Mollica, R. – National Academy for State Health Policy, Portland, ME
Assisted-care living facilities, otherwise known as assisted-living facilities, may also be referred to as residential care facilities for the elderly (In California, they are referred to as Residential Care Facilities). These facilities provide non-skilled care for people that need help with their activities of daily living but can also provide a lot of their own care and get through a daily routine with minimal assistance. Usually, skilled care is not provided in assisted-living facilities.
These facilities are an excellent alternative to a nursing home. The residents may live in individual apartments that they can furnish and personalize to make it seem more like home. Meals are usually provided in a community dining room and there are lots of activities and social events to attend. You can find these facilities as part of a larger independent retirement community, or as a stand alone facility that only offers assisted living. There are also small board and care homes that care for anywhere from 3-10 people. These are homes that have been converted to a board and care. Example: Veda was 87 years old and living in her own home. She was not getting out of the house and not socializing with anybody. Her daughter, Carol, arranged to have her mother move to an Assisted Living Facility after she realized that she was forgetting to take her medications and was not able to handle her own hygiene issues. She didn’t need skilled nursing care, but she did need help with her activities of daily living. Now Carol will not worry as much since there will be caregivers ensuring her mother gets her medications and assistance with her personal hygiene. Her mother will be able to participate in the weekly activities so she will remain active socially.
Adult Day Care
Adult day care is a community-based service that was developed to help keep people out of nursing homes and in their homes. Adult day care facilities offer custodial care during the weekdays (some provide weekend service). This care can be provided to people that need minimal assistance and have moderate impairments. Patients with Alzheimer’s or senile dementia are ideal candidates for this program.
Adult day care centers offer a form of support for those that live in their own homes, or maybe with their children. Adult day care centers offer family members who are providing care the much needed break during the day to continue to live their lives and provide care for their loved ones. Example: Marvin lives with his daughter, Kelly. Kelly works full time. Lately, she has noticed that Marvin has been forgetting to prepare and eat his meals during the day. One day she was called at work by a neighbor who found him wandering down the street. Kelly wants to take care of her father after work and on the weekends, but she needs help during the day. An adult day care would provide her with the solution she is looking for.
The costs of long-term care vary greatly depending on where you live and the type of care you receive. Many people think that home care usually costs less than nursing home care. However, skilled care at home can cost just as much, if not more than nursing home care. It depends on what type of care you need in your home, and for how many hours per day.
Here are Four Options To Pay For Your Long-Term Care
- You can rely on others (spouse, children, etc) to provide the help needed. This option is only available to those with a support system in place and if the amount and type of care required is possible for them to provide.
- You can self-insure and pay for your own long-term care with your own assets and income.
- You can spend down all of your assets and then qualify for Medicaid. (Medi-Cal in California).
- You can transfer a predetermined amount of risk of long-term care to an insurance company by purchasing long-term care insurance.
The cost of nursing home care can vary from close to $100 per day in the lower cost areas to almost $300 per day in a higher cost area. To summarize, the cost of nursing home care nationwide will run anywhere from about $32,900 to $149,700 per year (depending on where you live).
What will the future cost of long-term care be?
When planning for your future long-term care expenses it is important to not only note what the cost of care is today, but what it could be in the future. According to the General Accounting Office (1991), the annual cost of care is growing by 5.8% per year. This means that in 20 years the cost of long-term care could triple. So if you are 60 years old today, you needed care at age 80, and you lived in an area where the annual cost of care is $54,385.00 now, the cost in 20 years could be as much as $167,954.83. Imagine what your future expenses could be if you lived in a higher cost area!
Ancillary Costs
Besides the normal daily rate that a nursing home will charge you, or the hourly rate that a home care agency will charge you – there are always going to be ancillary costs you should plan for. In a nursing home, additional expenses could be diapers, laundry, medications, and other incidentals. In your home, there are additional expenses like safety devices (i.e. grab bars near the bathroom and toilet, and maybe a ramp for the stairs). “26.6% of the adult population has provided care for a chronically ill, disabled, or aged family member or friend during the past year. Based on current census data, that translates into more than 54 million people.”
Source: National Family Caregivers Association Random Sample Survey of 1000 Adults, Summer 2000
Human Costs
If a family member decides to provide the care rather than paying a professional, there are many human costs besides financial costs to consider. Your family may or may not be aware of these, or be prepared for them. If your plans are to save the expense of paying someone to care for you and rely on a family member instead, you need to consider the costs that they may pay – financially, physically, and emotionally.
Financial Costs
If you rely on family members to take care of you, it is important to consider the financial costs they may incur. They may be more than willing to take care of you, but may be unaware there may be a financial cost to them. The financial cost to them could be very high. If they currently work, they may need to work fewer hours, or even give up their jobs altogether. “The bulk of care giving is performed by women, and two-thirds of the caregivers are employed full or part-time.”
Challenged to Care: Informal Caregivers in a Changing Health System, Health Affairs, July/August 2002
Physical Costs
Providing long-term care is hard work. Family members may become exhausted from the long hours of care giving. If you had a stroke and could not bear your own weight it could be very difficult, if not impossible, for a family member to lift you in and out of bed. Especially if your caregiver were your spouse and you are both in your 80’s! If you have Alzheimer’s and require 24-hour care, it can be very exhausting for a family member to stay up all night and during the day. Your family caregiver couldn’t do that for too many days in a row!
Emotional Costs
The emotional toll caregivers experience is another cost your loved ones may pay in providing care to you. If you are relying on a family member to take care of you, it is important to understand the type of care you may be asking them to provide. You may be thinking that the extent of the care is helping you in and out of bed, assisting you with meal preparation, or driving you to the doctor. But, what if you need more care than that? Will it be possible for the friend or family member to handle more extensive care?
Unfortunately, private health insurance, Medicare, and Medicaid (Medi-Cal in California) are not realistic options to rely on to pay for your long-term care. This section addresses who pays for long-term care and what the limitations and disadvantages are in relying on those programs.
Department of Health and Human Services, CFA, Office of Actuary, National Health Statistics group, Personal Health Care Expenditures, 2001
Medicare
It is very important that you are aware of Medicare’s limits. Medicare may be one of the most misunderstood government programs in defining what is actually covered for long-term care services. Medicare is a federal program administered by the Center for Medicare and Medicaid. It is available to most people at age 65 or those with end stage renal disease.
According to the pie charts shown above, you can see that Medicare paid only a small percentage of the nation’s long-term care bill. The reason that Medicare doesn’t pay for more long-term care is that most long-term care is not skilled care and that is what Medicare primarily pays for. There are two parts to Medicare, Part A and Part B. As it relates to long-term care, Medicare Part A will pay for skilled nursing care, home health care (very limited), and hospice.
Medicare Skilled Nursing Facilities
Relying on Medicare to pay for your long-term care is not an adequate solution because it only has the potential to pay for up to 100 days in a skilled nursing facility. The requirement is that you have to be receiving skilled care on a daily basis at least five days a week and you have to have had a three-day hospital stay prior to entering the nursing home. Most people do not qualify for the entire 100 days because they don’t meet Medicare’s criteria. *There are additional criteria as well.
Medicare will pay for the first 20 days in full, and will pay for all costs except a co-pay in 2004 of $109.50 for the next 80 days. However, the average number of days paid by Medicare is only 23 days according to the Health Care Financing Administration, 1998.
It is important to point out that if you only needed custodial care you would not receive any Medicare benefits. Example: If you had Alzheimer’s disease and needed supervision, or if you needed help with your activities of daily living due to old age, these conditions would not qualify for Medicare benefits
Medicare Home Health Care Benefits
Many people mistakenly think that Medicare will pay for an unlimited amount of home care. Medicare will not pay for full-time long-term care. Medicare will only pay for a limited number of visits. The pie chart above shows you the percentages of the nation’s long-term care bill that covers home health care benefits. There are many requirements to get home health care benefits under Medicare. A few of them include that you must be homebound and must need skilled care for fewer than five days per week. In any case, Medicare generally does not adequately cover long-term care. For more information on Medicare you can call 1-800-Medicare (1-800-633-4227) to speak to a Medicare Customer Representative or visit http://www.medicare.gov
Common Misconceptions
If Medicare doesn’t pay, won’t my Medicare Supplement pay for my long-term care?
Generally, Medicare supplements only pay co-payments of Medicare. If Medicare will not pay for your care, then your Medicare supplement probably will not pay either.
I have an HMO, so doesn’t that pay for my long-term care?
Generally, HMO’s offer the same benefits that Medicare offers. To encourage people to assign their Medicare benefits to an HMO, many HMO’s offer additional ancillary benefits like vision and prescription benefits. However, they generally use the same criteria that Medicare does when it comes to paying for long-term care services.
Out of Pocket Expenses
If you do not qualify for Medicare or Medicaid to pay for your long-term care, then you have to pay long term care costs out of your own pocket. This may mean depleting your savings, cashing in your CDs, selling stocks and bonds, or even using cash value in a life insurance policy you may have. Unfortunately, for many people it does not take long before they deplete their hard-earned savings and end up qualifying for Medicaid (Medi-Cal in California).
Medicaid
Medicaid is a joint federal and state program that pays for medical care for individuals who cannot pay their own medical bills. (In California this program is known as Medi-Cal). To qualify for Medicaid, an individual must have limited income and few assets. Medicaid eligibility rules are complicated, and different states apply different rules. Each state operates its own Medicaid program, consistent with federal law.
Medicaid pays for a majority of our nation’s nursing home care costs. Unlike Medicare, Medicaid will pay for both skilled and custodial care, but in most cases is limited to nursing facility care. Medicaid pays for physician-approved hospital stays, medical care, prescription drugs, and skilled nursing home care. (There are exceptions in certain states)
The disadvantage to relying on Medicaid is that you will be very limited in your choices of nursing homes, or may be forced to go to a nursing home, since Medicaid usually does NOT pay for home care.
Income Limits
The income of a Medicaid nursing-home patient–usually Social Security and pension income–must generally be used to pay the costs of long-term care. The patient may keep a “personal-needs allowance” which averages $30 per month. (This varies by state.)
However, if the Medicaid nursing-home patient is married, the at-home spouse has the right to keep a certain amount of income, which can vary between $1,515.50 and $2,319. (This varies by state.) If the at-home spouse has income that is coming in their name alone, they are allowed to keep that income as well and it does not have to go toward their spouse’s long-term care costs.
Generally speaking, if the individual has enough income to pay for their own care they will not qualify for Medicaid even if they meet the asset requirements below. If a couple has enough income to provide the at-home spouse with the minimum income requirements and pay for the nursing home spouse’s long-term care, they will not qualify for Medicaid even if they meet the asset requirements.
Asset Limits
Before a Medicaid applicant can qualify for Medicaid they must “spend down” their assets, such as cash, stocks, and most other items with cash value, until around $2,000 remains. (This varies by state.)
If there is an at-home spouse, they may keep assets ranging between $18,552 and $92,760 depending on which state you live in. Any assets above that have to be “spent down”. This does not include the house and car and a few other assets. In determining Medicaid eligibility, the couple’s assets are evenly divided. The nursing home patient spends his/her half down to the state’s criteria, which averages around $2,000. (This varies by state.) The only way the at-home spouse can keep the maximum of $92,760 is if half of their assets are equal to or exceed the maximum of $92,760. If this is not the case, the at-home spouse will get to keep 50% of their assets. They are allowed to keep at least the minimum asset allowance in their state. There are a few states that automatically allow the at-home spouse to keep the maximum of $92,760 if the couple has that much in assets.
Transferring Your Assets to Qualify for Medicaid
Many people think a solution to qualify for Medicaid is to falsely impoverish themselves by giving their assets away. The 1993 budget bill (OBRA ’93) changed the transfer of asset guidelines to qualify for Medicaid’s nursing home benefit dramatically. This legislation requires the Medicaid program to “look back” 36 months (30 months for CA) prior to the application for Medicaid’s nursing home benefit to see if assets have been transferred for less than fair market value (i.e. to children or others). The look-back period is 60 months if assets were transferred to an irrevocable trust. The applicant is ineligible for the number of months equal to the amount of the transfer, divided by the state’s average cost of nursing home care.
Estate Recovery for Medicaid Benefits
Federal Law requires states to recover what was spent for the care at the death of the second spouse. State rules and practices for estate recovery vary significantly. Some states are stricter than others. In some states, placing a lien on your home is part of the estate recovery act.
Private Insurance
The percentage of long-term care paid for by private insurance includes both care paid for by individual and group long-term care insurance. It also includes care paid for by health insurance. For example, short-term rehabilitation after a car accident.
Other Public and Private Funds
There are other funds that can pay for long-term care, but they all have strict criteria and guidelines that must be met. An example would be the Veteran’s Administration. The Veteran’s health care benefits include medically necessary hospital and nursing home care and some outpatient care. The VA prioritizes veterans that qualify for care according to several categories. The first priority of veterans for receiving care is those veterans that have a service-connected disability. If you do not have a service-connected disability you are at the bottom of the priority list. There are income and asset requirements as well that must be met. To learn more about your eligibility benefits as a veteran, contact your local Department of Veterans Affairs Regional Office, or write to:
Veteran’s Benefits Department
Paralyzed Veterans of America
801 18th Street N.W.
Washington, D.C. 20006
Or call 800-424-8200
Save
Save